Antibiotic Resistance Risk Calculator
How Antibiotic Resistance Works
Before antibiotics, STIs were managed through suffering and isolation. The article explains how syphilis caused permanent damage without treatment, while today's antibiotics save lives but face new threats from overuse.
Historical Note: In 1943, penicillin cured a soldier with advanced syphilis in days. Now, we're seeing resistance develop in some gonorrhea strains, threatening to return us to the pre-antibiotic era.
Your Resistance Risk
Before antibiotics, people didn’t manage STI symptoms-they survived them. There were no quick fixes, no doxy-PEP, no 200 mg tablets to swallow after risky sex. If you had syphilis in 1890, you didn’t wait for a clinic visit. You waited. And you suffered. And often, you died.
The Reality of STIs Before Antibiotics
In the late 1800s and early 1900s, syphilis, gonorrhea, and chlamydia weren’t just infections-they were social disasters. A single sexual encounter could mean years of pain, disfigurement, or death. Syphilis, known as "the great imitator," could mimic almost any disease. It started with a painless sore, then a rash, then nerve damage, dementia, and heart failure. By the time it reached the tertiary stage, there was nothing doctors could do but watch. Gonorrhea, called "the clap," caused painful urination, pus discharge, and infertility. Women were especially vulnerable. Many never knew they had it until they couldn’t get pregnant. No tests existed. No antibiotics. No cure. Chlamydia was practically invisible. It didn’t always cause symptoms, so it spread silently. By the time someone realized something was wrong, damage was already done. Tubal scarring, ectopic pregnancies, chronic pelvic pain-these weren’t rare outcomes. They were expected.Treatments That Hurt More Than They Helped
Doctors tried everything. Mercury was the go-to for syphilis. Patients were rubbed with mercury ointments, inhaled mercury vapors, or given mercury pills. Some were even locked in mercury-filled rooms for days. The side effects? Excessive salivation, tooth loss, kidney failure, and brain damage. But it was better than the alternative: letting syphilis eat you alive. For gonorrhea, doctors used silver nitrate drops, caustic solutions, and even electric currents. Some tried bleeding patients or using arsenic-based drugs like Salvarsan, developed in 1910. Salvarsan was toxic, hard to prepare, and required multiple painful injections. It worked sometimes-but only if you survived the treatment. Women with STIs were often blamed. They were labeled "immoral," sent to "fallen women" asylums, or forced into quarantine. Men, especially those in the military, were treated more leniently. The double standard was brutal and widespread.How People Lived With STIs
Without cures, survival meant adaptation. People learned to recognize early signs: a sore that wouldn’t heal, unusual discharge, burning during urination. They avoided sex during outbreaks. Some turned to herbal remedies-goldenseal, garlic, witch hazel-none of which worked, but they offered a sense of control. Religious groups promoted abstinence. Public health campaigns focused on shame and fear. In 1914, the U.S. government launched the American Social Hygiene Association to "cleanse" society through moral education, not medicine. They distributed pamphlets warning of "the curse of lust," not bacteria. In urban centers, brothels often had their own "medics" who gave herbal washes or crude injections. In rural areas, people relied on folk healers, midwives, or prayer. Many just lived with it, hoping the symptoms would fade. Some did. Many didn’t.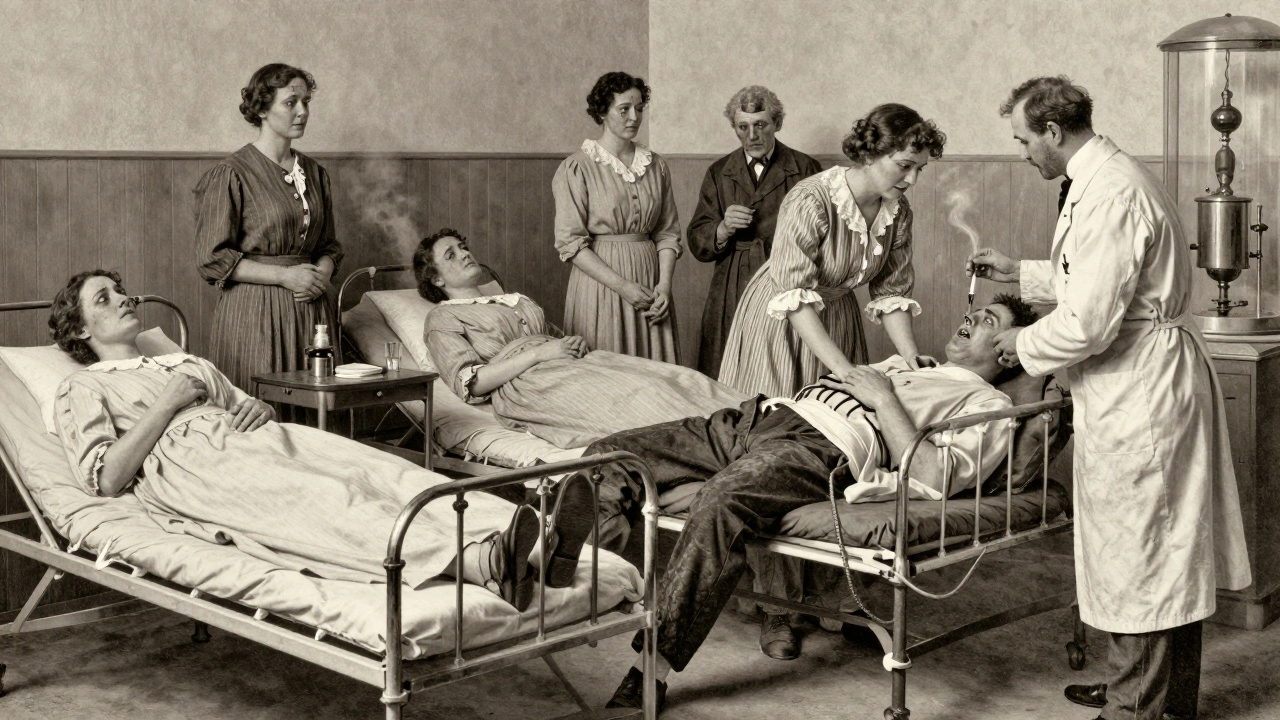
The Turning Point: Penicillin Changes Everything
Everything changed in 1943. Penicillin was mass-produced and used to treat a U.S. soldier with advanced syphilis. Within days, his sores vanished. Within weeks, he was healthy. By 1945, penicillin was widely available. The death rate from syphilis in the U.S. dropped by 85% in five years. Gonorrhea cases fell by half. Chlamydia, though still undiagnosed, became treatable once doctors realized it was bacterial. For the first time in history, STIs became curable. Not manageable. Not endured. Cured. This shift didn’t just save lives-it changed culture. Sex became less terrifying. Contraception and STI treatment gave people more control over their bodies. Public health efforts shifted from moral policing to medical care. The stigma didn’t disappear overnight, but it began to crack.Why "Pre-Antibiotic Care" Isn’t a Modern Concept
Today, some people talk about "pre-antibiotic care" as if it’s a new trend-something to do before taking antibiotics. But that’s a misunderstanding. There’s no such thing as managing an STI without a cure. Bacterial STIs like syphilis, chlamydia, and gonorrhea are curable. They always have been, since penicillin. What we see now-doxy-PEP-isn’t pre-antibiotic care. It’s antibiotic prophylaxis. It’s using antibiotics to prevent infection before it starts. It’s not about avoiding cures. It’s about using cures early to stop infections before symptoms appear. The idea of "managing symptoms without cures" belongs to the past. Today, we have tools. We have tests. We have antibiotics. The challenge isn’t finding ways to live with STIs. It’s using our tools wisely so we don’t lose them.




